What you should know:
– A new report speak Office of the National Coordinator for Health Information Technology (ONC) examines the current state of electronic health information exchange among hospitals in the United States. The results reveal progress in interoperability, but also highlight areas where improvements are needed.
– Furthermore, this Short describes the extent of electronic information exchange between hospitals and other providers across the care continuum and focuses on how often clinicians at these hospitals routinely use this information at the point of care.
Key takeaways
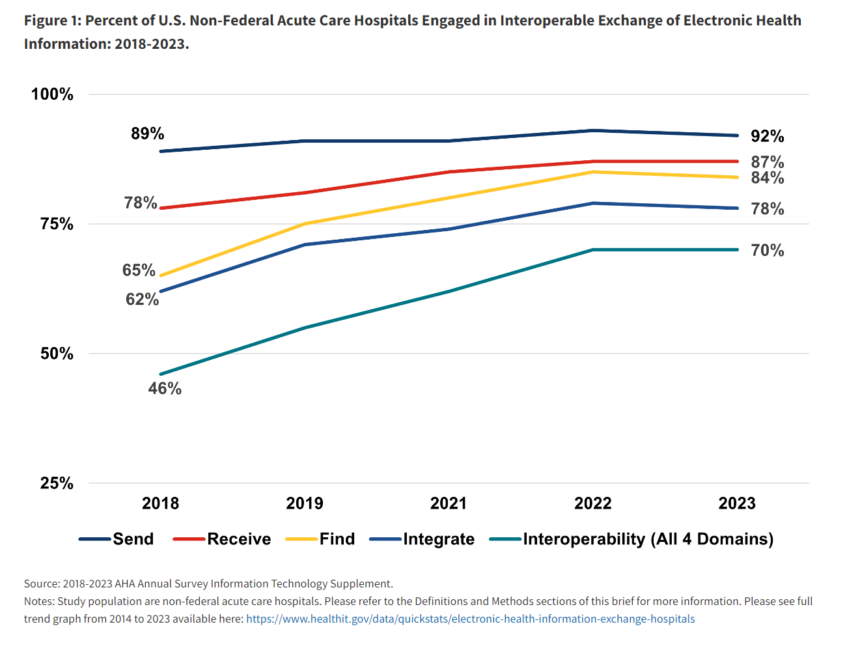
- Increased interoperability: The percentage of hospitals regularly engaging in all four areas of interoperable exchange (send, receive, find and integrate) has increased significantly since 2018, from 28% to 43% in 2023.
- Focus on routine exchanges: While most hospitals send health information electronically, only about three-quarters integrate the information they receive into their electronic health records (EHRs). The report highlights the importance of moving beyond “casual” exchange to “routine” exchange for optimal patient care.
- Resource disparity: Larger, urban, system-affiliated hospitals are more likely to engage in routine interoperable exchanges than smaller, rural, independent hospitals. This highlights the need for targeted efforts to support resource-constrained facilities.
- Data availability at the point of care: Hospitals that regularly exchange data have higher rates of clinician access and use of patient information from external providers at the point of care. This highlights the link between interoperability and improved care decisions.
- Limited exchange with certain suppliers: Despite progress, relatively few hospitals reported exchanging electronic care summaries with most long-term post-acute care (LTPAC) and behavioral health providers. This may reflect limitations in the data exchange capabilities of these providers.
The road ahead
The report suggests several key areas to focus on going forward:
- Encourage widespread routine exchange: Continued efforts are needed to promote the move from “casual” to “routine” interoperable exchanges across all healthcare settings.
- Fight against disparities: Initiatives should be implemented to bridge the gap in interoperability capabilities between different types of hospitals.
- Extension of data exchange: Efforts are needed to improve data exchange with LTPAC and behavioral health providers to ensure a more comprehensive view of patient care.
Although hospitals have made significant progress in interoperable data sharing, additional work is needed to achieve regular, nationwide exchange across the entire health care continuum. By focusing on these key areas, stakeholders can ensure that all patients benefit from improved care coordination and decision-making through seamless data exchange.